
Like us! Follow us! Share us! View us!
Did you know that W.O.M.E.N. is on Facebook, Twitter and YouTube? From important information to new services, to exciting events and the latest news – you can have all the information at your fingertips daily just by the click of a mouse! We are so proud of all of the exciting things we have going on and are excited to be able to share it right to your newsfeed!
Make W.O.M.E.N. part of your day and get up to date information that is vital to your everyday life!
“LIKE” us on Facebook at www.facebook.com/EducatingWomen
“FOLLOW” us on Twitter at www.twitter.com/Educating-Women
“WATCH” us on YouTube at www.youtube.com/EducatingWOMEN
We want to know what YOU think! Make sure to leave us comments and and let us know what you want to see!
Ever feel clueless when it comes to HIV lingo?
Never fear! Click the image below to go to Healthline’s website where you can hover over the words to see their definitions!
 |
>
Source: http://www.healthline.com/health/hiv-aids/words-you-should-know (2014)

Understanding Triple Negative Breast Cancer
Did you know that there is not just one form of Breast Cancer? In fact, today, there are many different “subtypes” of Breast Cancer. These subtypes of Breast Cancer are generally diagnosed based upon the presence, or lack of, three “receptors” known to fuel most breast cancers: estrogen receptors, progesterone receptors and human epidermal growth factor receptor 2 (HER2). The most successful treatments for breast cancer target these receptors.
Unfortunately, when it comes Triple Negative Breast Cancer, none of these receptors are found in women who are diagnosed. In other words, According to the Triple Negative Breast Cancer Foundation, a triple negative breast cancer diagnosis means that the offending tumor is estrogen receptor-negative, progesterone receptor-negative and HER2-negative, thus giving rise to the name “triple negative breast cancer.” On a positive note, this type of breast cancer is typically responsive to chemotherapy. Because of its triple negative status, however, triple negative tumors generally do not respond to receptor targeted treatments. Depending on the stage of its diagnosis, triple negative breast cancer can be particularly aggressive, and more likely to recur than other subtypes of breast cancer.
Age, Race or Ethnicity: Several studies suggest that being pre- menopausal, African-American, Latina or Caribbean increases your risk of developing basal-like or triple-negative breast cancer. Among African-American women who develop breast cancer, there is an estimated 20 to 40 percent chance of the breast cancer being triple-negative. Researchers do not yet understand why premenopausal women and women in some ethnic groups have higher rates of triple- negative breast cancer than other groups of women.
Source: Guide to Understanding Triple Negative Breast Cancer
Researchers are still learning why some women are more likely than others to develop triple-negative breast cancer. Research supports a relationship between risk and your genes, age, race and ethnicity.
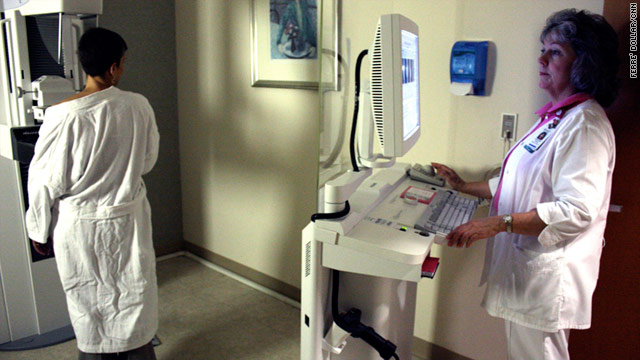
6 Things to Know about Mammograms
A mammogram is an important step in taking care of yourself and your breasts. The American Cancer Society recommends women age 40 and over get a mammogram every year, along with a breast exam by a doctor or nurse. Below are 7 things we think you should know before going for a mammogram to make the visit as comfortable as possible.
1. What is a mammogram?
A mammogram is an x-ray of the breast that’s used to find breast changes. The x-rays used for mammograms produce lower energy x-rays and expose the breast to much less radiation compared with those in the past.
2. Where do you get a mammogram?
Find a center in your area that specializes in mammograms. The US Food and Drug administration certifies mammogram facilities that meet high professional standards of quality and safety. Having all your mammograms at the same facility will make it easier for doctors to compare images from one year to the next.
3. When is the best time to schedule a mammogram?
The best time to schedule your mammogram is about one week after your menstrual period. Your breasts won’t be as tender or swollen, which means less discomfort for you.
4. What do I wear to a mammogram?
It is best to wear a two-piece outfit because you will need to remove your top and bra. Do not apply deodorant, antiperspirant, powder, lotion, or ointment on or around your chest on the day of your mammogram. These products can appear as white spots on the x-ray.
5. What to expect
The entire procedure takes about 20 minutes. The breast is compressed between two plastic plates for a few seconds while an x-ray is taken. It is repositioned (and compressed again) to take another view. There is no denying this process is uncomfortable, but it is necessary to get the clearest view.
6. Getting the results
You should get your results within 30 days of your mammogram. If you don’t, you should call your doctor to ask about your results. If the doctor finds something suspicious, you will likely be contacted within a week to take new pictures or get other tests. This does not mean you have Breast Cancer, it may be dense breast tissue or a cyst, or maybe that the image just isnt clear enough.

Breast Cancer: Myths & Facts
Between our peers, magazines, newspapers and the internet, we are flooded with information regarding Breast Cancer. Sometimes, it can be a bit overwhelming, but with the help of the National Breast Cancer Foundation, Inc., we thought it would be important to share some of the most common myths and facts regarding Breast Cancer.
Myth: Finding a lump in your breast means you have Breast Cancer
Fact: Only a small percentage of breast lumps turn out to be cancer. But if you discover a persistent lump in your breast or notice any changes in breast tissue, it should never be ignored. It is very important that you see a physician for a clinical breast exam. He or she may possibly order breast imaging studies to determine if this lump is of concern or not. Make sure to click HERE to see how to perform your own breast exam at home!
—————————————————————————————————————————————————————————————
Myth: A mammogram can cause breast cancer to spread
Fact: A mammogram currently remains the highest standard for the early detection of breast cancer. Breast compression while getting a mammogram cannot cause cancer to spread. According to the National Cancer Institute, “The benefits of mammography, however, nearly always outweigh the potential harm from the radiation exposure. Mammograms require very small doses of radiation. The risk of harm from this radiation exposure is extremely low.”
—————————————————————————————————————————————————————————————
Myth: If you have a family history of Breast Cancer, it is likely you will develop Breast Cancer
Fact: While women who have a family history of breast cancer are in a higher risk group, most women who have breast cancer have no family history. Statistically only about 10% of individuals diagnosed with breast cancer have a family history of this disease.
—————————————————————————————————————————————————————————————
Myth: Breast Cancer is contagious
Fact: You cannot catch breast cancer or transfer it to someone else’s body. Breast cancer is the result of uncontrolled cell growth of mutated cells that begin to spread into other tissues within the breast.
—————————————————————————————————————————————————————————————
Myth: Deodorant causes Breast Cancer
Fact: Researchers at the National Cancer Institute (NCI) are not aware of any conclusive evidence linking the use of underarm antiperspirants or deodorants and the subsequent development of breast cancer.
—————————————————————————————————————————————————————————————
REMEMBER: You know your body better than anyone else, if you feel something is not normal with your body, it is imperative to see your doctor as soon as you can.

October is Breast Cancer Awareness Month
W.O.M.E.N. is going PINK for Breast Cancer Awareness Month! Throughout the month of October, we will be sharing important information vital to every woman’s health. There is no better time than now to take the best care of your body you possibly can and we hope to help you every step of the way.
The first step in being proactive regarding Breast Health can be done in the comfort of your own home, a Breast Self-Exam. A woman is suggested to perform a Breast Self-Exam once a month. Johns Hopkins Medical center states, “Forty percent of diagnosed breast cancers are detected by women who feel a lump, so establishing a regular breast self-exam is very important.” While mammograms can help you to detect cancer before you can feel a lump, breast self-exams help you to be familiar with how your breasts look and feel so you can alert your healthcare professional if there are any changes. How should a self-exam be performed? Below are some tips for performing a Breast Self-Exam at your convenience.
In the Shower: Using the pads of your fingers, move around your entire breast in a circular pattern moving from the outside to the center, checking the entire breast and armpit area. Check both breasts each month feeling for any lump, thickening, or hardened knot. Notice any changes and get lumps evaluated by your healthcare provider.
In front of a mirror: Visually inspect your breasts with your arms at your sides. Next, raise your arms high overhead. Look for any changes in the contour, any swelling, or dimpling of the skin, or changes in the nipples. Next, rest your palms on your hips and press firmly to flex your chest muscles. Left and right breasts will not exactly match—few women’s breasts do, so look for any dimpling, puckering, or changes, particularly on one side.
Lying Down: When lying down, the breast tissue spreads out evenly along the chest wall. Place a pillow under your right shoulder and your right arm behind your head. Using your left hand, move the pads of your fingers around your right breast gently in small circular motions covering the entire breast area and armpit. Use light, medium, and firm pressure. Squeeze the nipple; check for discharge and lumps. Repeat these steps for your left breast.
Can you rely on self-exams alone to make sure you are cancer free? Remember, mammograms can detect tumors before they can be felt, so screening is key for early detection. But when combined with regular medical care and appropriate guideline-recommended mammography, breast self-exams can help women know what is normal for them so they can report any changes to their healthcare provider. If you find a lump, schedule an appointment with your doctor, but don’t panic — 8 out of 10 lumps are not cancerous. For additional peace of mind, call your doctor whenever you have concerns.
W.O.M.E.N. has individual Brest Self-Exam cards in our office, which are free to the public! Can’t make it to the office? Just send us your information and we will be happy to send a card to you or your loved one.

Ovarian Cancer – Signs and Symptoms
It is always important to pay attention to your body and know what is normal for you from head to toe. It is especially important for women to pay attention to certain gynecologic signs that may be abnormal. Those signs may be your body telling you something is seriously wrong. According to the Ovarian Cancer National Alliance, The American Cancer Society estimates that in 2013, about 22,240 new cases of ovarian cancer will be diagnosed and 14,030 women will die of ovarian cancer in the United States. A woman’s lifetime risk of developing invasive ovarian cancer is 1 in 72 and a woman’s lifetime risk of dying from invasive ovarian cancer is 1 in 95.
According to the Centers For Disease Control, Ovarian cancer may cause one or more of these signs and symptoms—
- Vaginal bleeding or discharge from your vagina that is not normal for you.
- Pain in the pelvic or abdominal area (the area below your stomach and between your hip bones).
- Back pain.
- Bloating, which is when the area below your stomach swells or feels full.
- Feeling full quickly while eating.
- A change in your bathroom habits, such as having to pass urine very badly or very often, constipation, or diarrhea.
Research suggests that the majority of women with ovarian cancer experience symptoms. Symptoms vary and often depend on the location of the tumor and its impact on the surrounding organs. Many ovarian cancer symptoms mimic those of less life-threatening conditions such as irritable bowel syndrome which makes it even that much more important to see a doctor if you are experiencing any of the above mentioned symptoms.

When Faced with Resistance…
When faced with resistance, apply persistence!

HIV/AIDS and Aging
HIV/AIDS and aging were not usually two words that went together. When the epidemic first began to spread, those who were diagnosed were not expected to live much longer. Fortunately,with new medications and treatments, the life expectancy of someone living with HIV/AIDS has increased drastically which makes aging with HIV/AIDS a reality all over the world. In fact, almost one-fourth of people living with HIV/AIDS in our world today are over the age of 50. Living with HIV presents certain challenges, no matter what your age. Yet, older Americans with HIV may face different issues than their younger counterparts, including greater social isolation and the lack of a strong, local support system. Older individuals may also face different stigmas when disclosing their status to partners, family, or friends. Aging normally is associated with a myriad of risks including anything from arthritis to osteoporosis. Yet, complications can arise and illnesses can be worsened with aging and HIV. Some of those specific illnesses include Dementia, Depression, High Cholesterol, and Infections to name a few.
In all actuality, there may even be many more cases today than we know about. Why? One reason may be that doctors do not always test older people for HIV/AIDS and so may miss some cases during routine check-ups. Another may be that older people often mistake signs of HIV/AIDS for the aches and pains of normal aging, so they are less likely than younger people to get tested for the disease. Also, they may be ashamed or afraid of being tested. People age 50 and older may have the virus for years before being tested. By the time they are diagnosed with HIV/AIDS, the virus may be in the late stages.
The number of HIV/AIDS cases among older people is growing every year because:
1. Older Americans know less about HIV/AIDS than younger people do. They do not always know how it spreads or the importance of using condoms, not sharing needles, getting tested for HIV, and talking about it with their doctor.
2. Healthcare workers and educators often do not talk with middle-aged and older people about HIV/AIDS prevention.
3. Older people are less likely than younger people are to talk about their sex lives or drug use with their doctors.
4. Doctors may not ask older patients about their sex lives or drug use or talk to them about risky behaviors.
Remember, W.O.M.E.N. offers FREE and CONFIDENTIAL HIV testing as well as counseling services. There is no reason, especially age, to not stop by and know your status.






